Poster Presentation Australian Diabetes Society and the Australian Diabetes Educators Association Annual Scientific Meeting 2016
The high frequency and frequent variations of inpatient hyper- and hypoglycaemia in a large teaching hospital. (#380)
Rates of in-patient diabetes are reported to be in the order of 11‐25%. Both in-patient hypoglycaemia and hyperglycaemia are associated with excess morbidity and mortality, during admission and post-discharge. Many hospitals have treatment protocols in place for in-patient glucose management based on bedside capillary blood glucose (CBG) monitoring. We examined the frequency of blood glucose monitoring and the burden of meter recorded hyper- and hypoglycaemia in a convenience sample of medical and surgical wards at RPAH. In addition, ward nursing staff were randomly selected to complete a diabetes knowledge questionnaire.
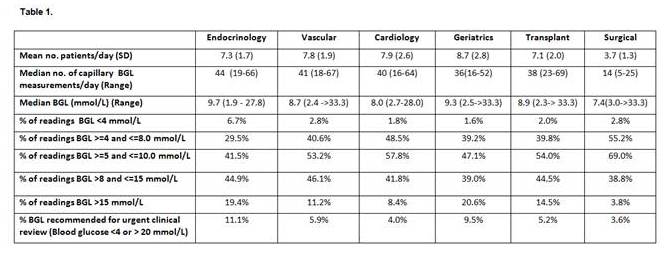
De-identified CBG results were downloaded weekly from blood glucose meters from six wards over five consecutive weeks. The number of patients with diabetes per ward, per day was ascertained. A total of 7839 capillary glucose measures were available for analysis. Overall, 48.3% of CBG levels were outside the target 5 to 10 mmol/L range. In-patient hyperglycaemia is common with 40% of readings above the target range. 17.2 % of readings were <4 or >15mmol/L. Both hyper- and hypoglycaemia were more frequent on the Endocrine ward (Table 1) perhaps reflecting the cause of admission, however the severity of hyperglycaemia detected appeared to be greater in surgical, transplant and geriatric wards (including CBG>33.3mmol/l). Conversely, hypoglycaemia was a much less common event across most wards. Only one glucose measurement of <2.2 mmol/l was recorded. However, there was considerable variation in hypoglycaemia knowledge; of concern 30% of nurses surveyed were uncertain about appropriate treatment of severe hypoglycaemia. A hypo kit was also absent from one ward.
Hyperglycaemia still appears to be a very frequent in-patient finding. These data suggest that there is scope and opportunity to improve in-patient diabetes management with respect to both staff education and glycaemic management protocols to improve in-hospital and post discharge outcomes.