Poster Presentation Australian Diabetes Society and the Australian Diabetes Educators Association Annual Scientific Meeting 2016
An evaluation: Educating primary healthcare nurses in general practice to better manage patients with diabetes (#381)
Background: Diabetes has become the highest burden of disease in Australia, with Western Sydney (WS) identified as a diabetes hotspot. The WS Diabetes initiative is building the capacity of general practice to enhance the management of type 2 diabetes through specialist/GP case conferences, HealthPathways, Integrated Care, and GP phone support lines. We recognised that primary healthcare nurses (PN) are ideally placed to provide self-management education, but many reported they need further education with cost and time cited as barriers.
Aim: To improve PN knowledge and confidence to provide basic diabetes self-management education and enhancing diabetes management in primary care.
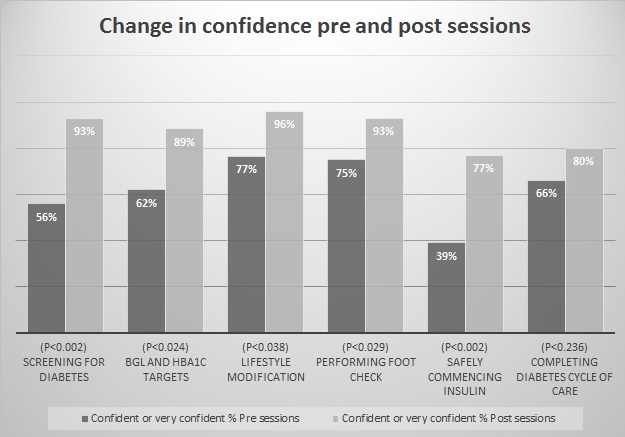
Methods: Four education sessions of two hours duration each were delivered over 6 weeks. Each session consisted of 3-5 presentations. Promotion and registration was through WSPHN. 48 PNs registered from 26 different practices. 26 attended all 4 sessions and 30 completed a pre course needs assessment. A questionnaire to assess PN confidence to manage diabetes was conducted before the first session and on completion of session 4. Topics were: ‘Screening for diabetes’, ‘Targets for diabetes’, ‘Lifestyle modification’, ‘Foot checks’, ‘Commencing insulin’, ‘Diabetes cycle of care’. Responses were rated from ‘1’ (not-at-all confident) to ‘4’ (very confident).
Findings: Post confidence assessment showed statistically significant improvement, averaging 25.5% in feeling ‘confident’ or ‘very confident’ across all topics (pre-62.5%: post-88%) except ‘Diabetes cycle of care’. Amongst PNs reporting feeling ‘not at all confident’, an average of 14% decrease was seen (pre-15%: post-0.6%).
Discussion: The sessions were highly appreciated and effective at improving PN confidence in key areas of diabetes education. This is a novel way of building primary care capacity to manage diabetes. The sessions will be repeated annually using a similar format with some key sessions made available online providing flexibility and convenience to PN who are unable to attend the sessions.